|
|
 |
Back to 2011 Program
Free flap take-back following postoperative microvascular compromise: predicting salvage versus failure
Michael N. Mirzabeigi, MS, Theresa Wang, MD, Stephen J. Kovach, MD, David W. Low, MD, Jesse A. Taylor, MD, Joseph M. Serletti, MD, Liza C. Wu, MD.
University of Pennsylvania, Philadelphia, PA, USA.
BACKGROUND: Postoperative microvascular compromise remains an infrequent yet devastating complication following free tissue transfer. Optimal perioperative strategies for achieving a successful take-back have yet to be elucidated. As attempted salvage is both a relatively uncommon occurrence as well as a technically complex endeavor, limited clinical data has come forth to supplant questions surrounding successful free flap salvage. The purpose of this study is twofold: 1) to stratify preoperative risk factors that predict the success of a take-back 2) to identify perioperative strategies that correlate with successful salvage.
METHODS: A retrospective chart review was performed on all free flaps performed from January 2005 - April 2011. All flaps were monitored by means of conventional clinical indicators (ie color, temperature, capillary refill, turgor) and hand-held Doppler ultrasonography. Buried flaps were monitored via an implantable Doppler system. The time until salvage was defined as the end of the initial procedure until the initiation of the salvage attempt. The primary endpoint, successful salvage, was defined as any flap that did not result in total loss. Univariate statistical analyses included Fisher’s exact test and the Mann-Whitney U test, in addition to binary logistic regression for multivariate significance. A value of p<0.05 was utilized to determine statistical significance. All statistical analysis was performed using SPSS for Windows version 18.0 (SPSS, Inc., Chicago, Ill.).
RESULTS: A total of 47 take-backs for delayed microvascular compromise were identified. Preoperative factors were then examined among those flaps which were salvaged versus those which ultimately failed. Following univariate analysis, the mean time until take-back, presence of thrombophilia, and mean platelet counts were significant factors predictive of unsuccessful salvage.(Table 1) A multivariate analysis was performed in which platelet counts remained significant (p = 0.05)
Of the 47 flaps, 11 flaps were not felt to be salvageable in the early stages of re-exploration during the take-back. Therefore, these flaps did not undergo a full-fledged salvage attempt and were excluded from further analysis. As a subgroup, the remaining 36 flaps that underwent salvage maneuvers were examined for both preoperative and intra-operative factors which could potentially predict success. Following univariate analysis of this subgroup, surgeon experience (defined as >5 yrs in practice) was the only factor that remained significant; however, intra-operative heparin anticoagulation and complete mechanical removal of a thrombus trended toward significance.(Table 2)
CONCLUSIONS: This study represents one of the largest take-back series in the published literature. Although further validation is necessary, there is evidence to suggest that there may be preoperative factors that are predictive of flap salvage success, including routine laboratory platelet values. Shorter time to take-back and surgeon experience may improve salvage while intraoperative heparin anticoagulation and complete mechanical removal of the thrombus demonstrate preliminary evidence as effective intraoperative strategies. 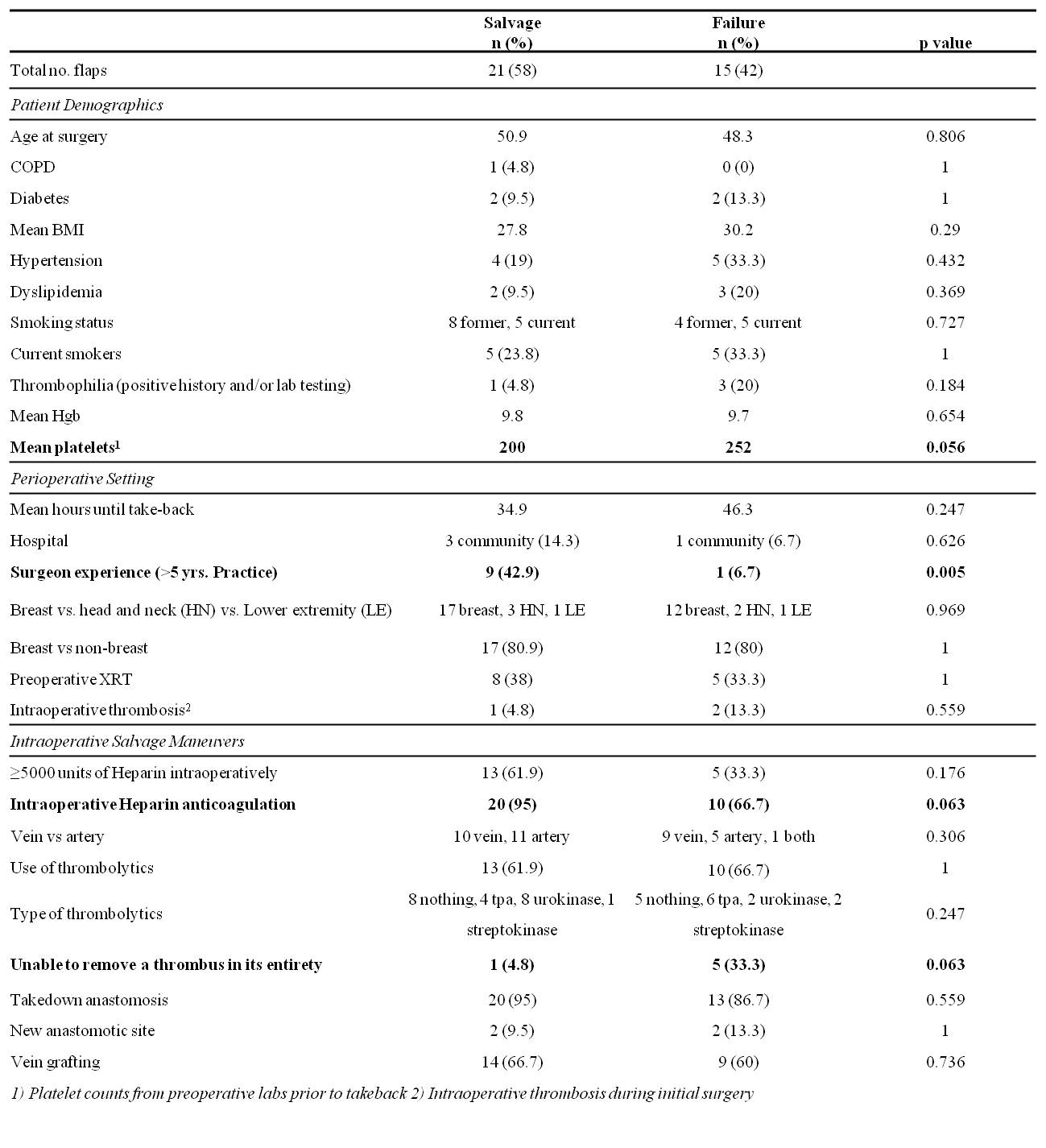
Back to 2011 Program
|








