|
|
 |
Back to 2011 Program
Allegations and Outcomes: A ten year analysis of surgery liability claims.
Bryson G. Richards, M.D., Spencer Studwell, J.D., John A. Girotto, M.D., M.M.A..
University of Rochester Medical Center, Rochester, NY, USA.
BACKGROUND -
During the national debate on health care, the impact of medical liability on the overall cost of care has emerged. Indemnity payments awarded to patients total approximately 5.72 billion annually. The University of Rochester Medical Center (URMC) is a tertiary referral center in western New York. This study reviews malpractice claim data at our institution over the last 10 years (2000-2009). Plastic Surgery claims are separately examined.
METHODS-
A retrospective review was conducted of malpractice claims against URMC surgical services and anesthesia providers excluding obstetrics. From each filed claim, our liability group summarized the specific data and created a case review abstract. Emphasis is placed on the respective intuitional costs for each outcome, allegation, and contributing factor.
RESULTS-
Over a ten year period, an estimated 250,000 procedures at our institution has led to 162 malpractice claims with $44 million total liability incurred. 41 claims are still in litigation. The average cost per closed claim was $251,000. High, moderate, and low injury severities made up 32%, 60%, and 8% of claims with average costs of $574,000, $110,000, and $7,200 respectively. Injury leading to a return trip to the OR accounted for 47% of claims, 75% of costs (average $412,000). Of closed claims, 37 yielded less than $10,000, and only 10 “mega” awards provided payments of $1 million or more.
A list of contributing factors for each claim was assigned by the insurer. Most commonly identified, intra-operative technical error and improper post-surgical monitoring was involved in 24% and 13% of claims respectively, combining to entail 58% of total cost. The dollar enumeration directly related to number of contributing factors recognized: average cost of $25,000 if no factors were cited, $114,000 if only one factor, and $1.4 million if more than 4 contributing factors were identified.
We have seen a trend in decreased annual frequency of claims. Annual liability costs are presented in this chart:
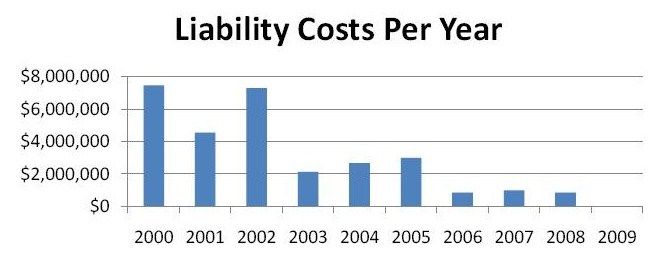
Few claims were asserted against URMC Plastic Surgeons, incurring a total cost of $24,956 (<0.001% of total cost). One claim is still in litigation. No claims were made for alleged technical error, improper surgical management, or by patients “dissatisfied” with surgical results. No claims have been filed against the plastic surgery providers for events during the most recent 5 years.
CONCLUSIONS-
From case review abstracts provided by the liability insurer, we saw increased liability costs for care that resulted in: high severity injury, return to the operating room, and injury from multiple contributing factors. Liability from plastic surgery claims was small. Since 2000, new initiatives to reduce medical errors have been implemented by an active Chief Quality Officer. These include: new CEO leadership with safety as their top agenda item, accountability through weekly “harm reports,” and Board Level Safety Committee meetings. We believe this reflects a trend toward decreased annual liability claims and costs at our institution since 2000.
Back to 2011 Program
|








