|
|
 |
Back to Annual Meeting Program
Comparison of irradiated versus non-irradiated DIEP flaps in patients undergoing immediate bilateral DIEP flap reconstruction and unilateral post-mastectomy radiation
Emily M. Clarke-Pearson, MD1, Manjeet Chadha, MD1, Joseph H. Dayan, MD1, William Sampson, MD2, Mark Sultan, MD2, Susan K. Boolbol, MD1, Mark L. Smith, MD1.
1Beth Israel Medical Center, New York, NY, USA, 2St. Luke's/Roosevelt Medical Center, New York, NY, USA.
Background
Patients with locally advanced breast cancer desiring DIEP flap reconstruction may also need post-mastectomy radiation therapy (PMRT). In this setting, surgeons often advocate delaying the DIEP reconstruction until after PMRT is finished to avoid negative effects on the flap. Drawbacks to this approach include additional surgery, recuperation, and cost, as well as an extended period of asymmetry. In addition, it is more difficult to re-establish the preoperative proportions of the skin envelope, even if a tissue expander is employed. We therefore offer primary reconstruction with DIEP flaps to patients who may require PMRT. We review the outcomes of patients undergoing bilateral DIEP flap reconstruction who received unilateral PMRT by comparing irradiated versus non-irradiated flaps in the same patient.
Methods
125 patients who underwent immediate DIEP reconstruction between 2009 and 2011 were identified (62 bilateral and 63 unilateral). 11 consecutive patients had bilateral DIEP reconstructions by a single surgeon and received unilateral PMRT. Magnetic resonance angiography was used preoperatively to identify the dominant perforators. The flaps were then aggressively trimmed to leave only well-vascularized tissue. Additionally, buried portions were de-skinned, removing both the epithelial and dermal layers, to decrease fibrous elements that might contribute to contracture after radiation. These patients received 50.4 Gy radiation delivered to the reconstructed mound in a standard three-beam fashion. Results were documented photographically. Using the contralateral, non-irradiated breast as a control, the complication rates, incidence of clinically significant fat necrosis, and need for reoperation were examined.
Results
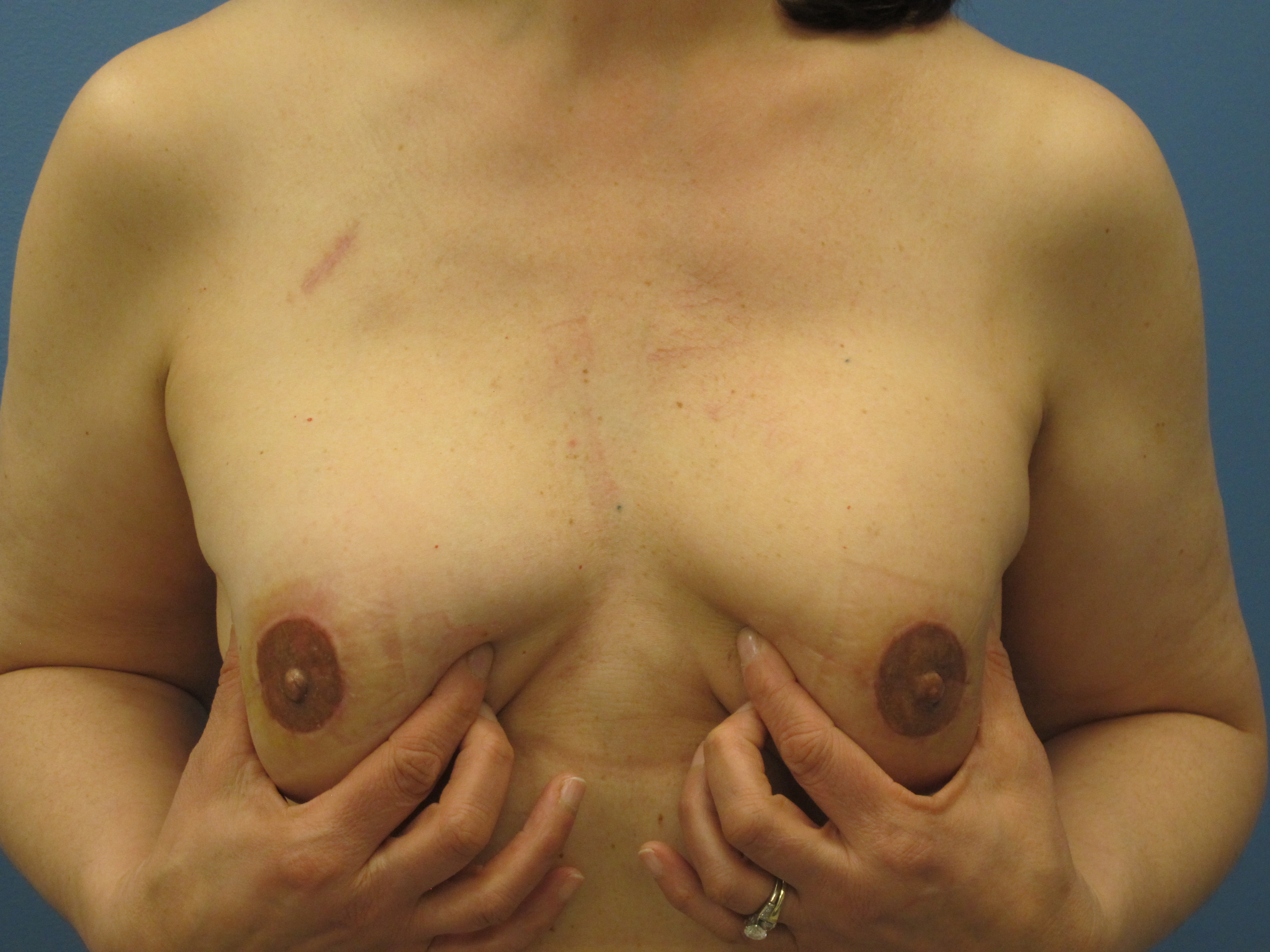
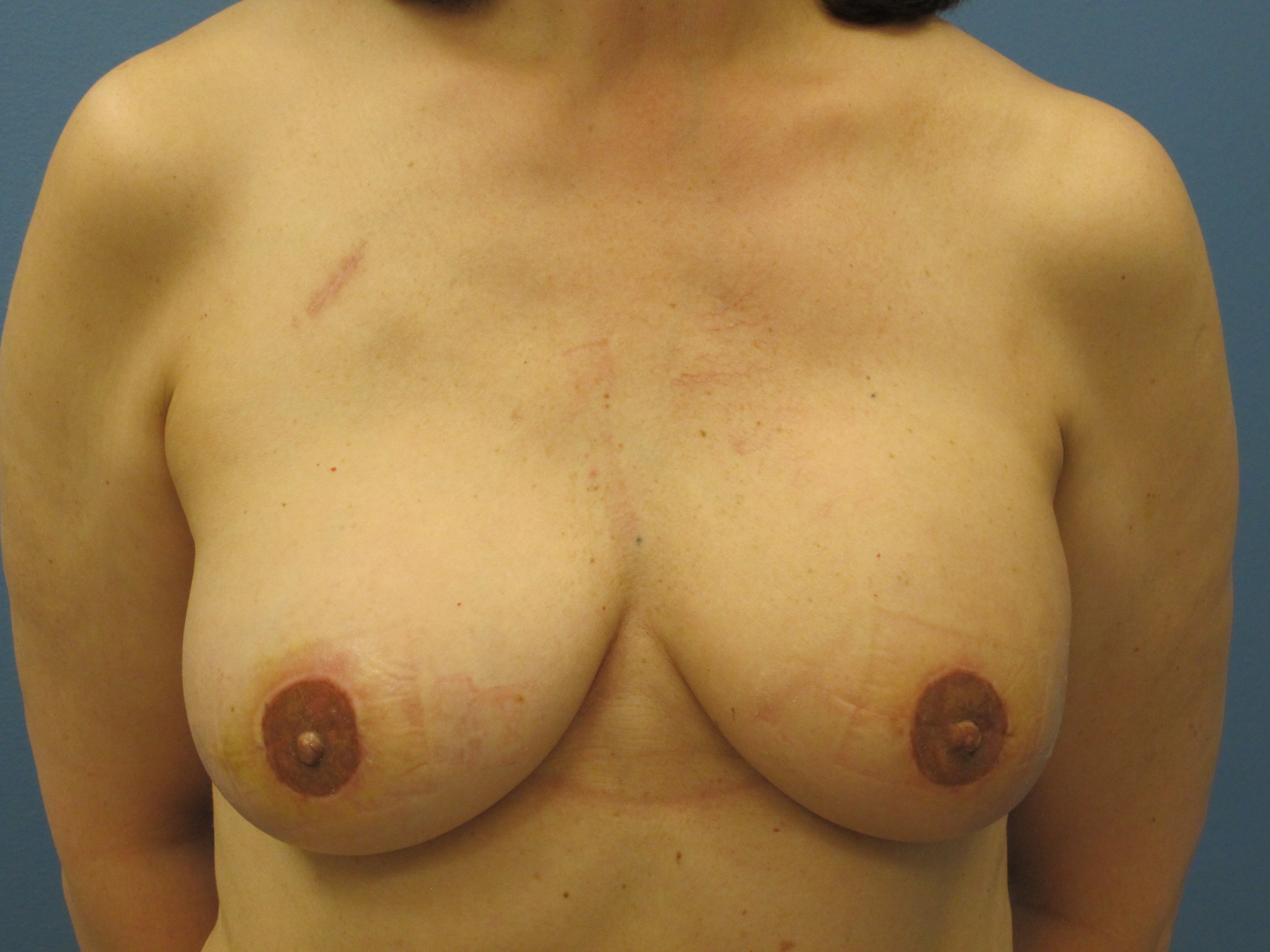
Median follow-up was 18 months (range 8 - 21 months). There was no incidence of clinically significant fat necrosis in either the irradiated or non-irradiated DIEP flaps. (Fig. 1) Complications occurring prior to PMRT included two patients with minor wound breakdown requiring wound care. Following PMRT, one patient had CTC grade 3 skin toxicity, and one had delayed healing of a nipple reconstruction. Both healed with conservative treatment. Operative revision for breast symmetry, not including nipple areola reconstruction or tattooing, was required in three of the eleven patients. In these cases, revisions were performed on both breasts to address the asymmetry. Aesthetic outcomes were deemed satisfactory in all patients. (Fig. 2)
Conclusions
Primary reconstruction with DIEP flaps can be performed successfully in patients who require post-mastectomy radiation therapy. Patients achieved a natural breast mound at the time of mastectomy with optimal preservation of the breast skin envelope.
Back to Annual Meeting Program
|








