|
|
 |
Back to Annual Meeting Program
A 15-year Experience with Complex Scalp Reconstruction Using Free Tissue Transfer: Analysis of Risk Factors for Complications
Brady Sieber1, John P. Fischer, M.D.2, Jonas A. Nelson, M.D.2, Stephen J. Kovach, M.D.2, Scott P. Bartlett, M.D.2, Joseph M. Serletti, M.D.2, Jesse A. Taylor, M.D.2, Suhail Kanchwala, M.D.2, David W. Low, M.D.2.
1University of Pennsylvania School of Medicine, Philadelphia, PA, USA, 2Hospital of the University of Pennsylvania, Philadelphia, PA, USA.
Background:
Large, complex scalp defects represent a significant reconstructive challenge. Thus, a variety of free flap techniques have been used to provide optimal soft tissue coverage of scalp wounds. The goal of this study is to report a large experience of free tissue transfers for scalp defects and to determine risk factors associated with complications.
Methods:
A retrospective review of free tissue transfers for scalp defects from 1997-2011 was performed. Endpoints included patient co-morbidities, defect characteristics, flap choice, and post-operative complications. A multivariate analysis was performed to determine significant predictors of complications. Subgroup analyses compared antero-lateral thigh (ALT) to latissimus dorsi (LD) flaps and immediate cranioplasty with free flap to no cranioplasty.
Results:
Over the 15-year study period, 43 flaps were performed in 37 patients with a success rate of 98 percent. Our study group included patients with: prior scalp surgery (81 percent), XRT (55 percent), smoking (35 percent), and immediate cranioplasty (24 percent). Flaps used for coverage, included: ALT (n=17), LD (n=16), DIEP/TRAM (n=4), para-scapular (n=2), and other (n=4). Multivariate analysis demonstrated defect size (298 cm2 versus 173 cm2, p=0.048) and smoking (56 percent versus 27 percent, p=0.05) were associated with significant wound complications. Additionally, HTN (33 percent versus 25 percent, p < 0.0001) and DM (19 percent versus 25 percent, p < 0.0001) were predictors of major postoperative complications (flap loss, re-exploration, intra-cranial infection, and complete flap atrophy).
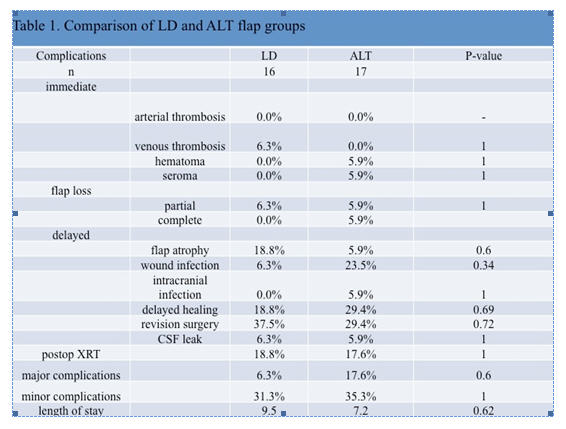
We compared LD (n=16) and ALT (n=17) flaps and found no differences in complication rates between groups (Table 1). Recipient vessel choice did tend to differ with the superficial temporal being used for LD flaps and facial for ALT flaps (p=0.07). Immediate cranioplasty with free tissue transfer was performed in 10 patients with 100 percent success. In comparing the cranioplasty group to all other patients, there was no difference in CSF leak, thrombotic or wound complications. Cranioplasty increased OR time (592 vs. 495 min, p = 0.019), EBL (750 vs. 341 cc, p = 0.047), and transfusion rates (56% vs. 16%, p = 0.045).
Conclusions:
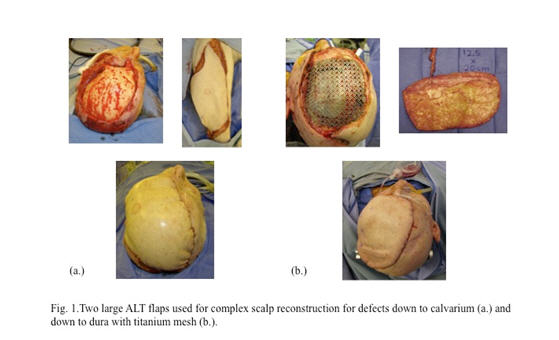
We report a 98 percent reconstructive success rate in managing large, complex scalp defects in high-risk patients, and provide the largest head-to-head comparison of ALT and LD flaps to date. Our data show that LD and ALT flaps are equally safe and efficacious, but we have preferentially shifted our use toward ALT given its versatility (Figure 1). We report that both defect characteristics (size of wound) and patient factors (smoking, HTN, and diabetes) are significant predictors of postoperative complications and must be considered when evaluating and counseling patients regarding risk. Immediate cranioplasty was also successfully performed for large calvarial defects, however these patients must be cautiously selected due to added operative time and blood loss.
Back to Annual Meeting Program
|








