|
Back to Annual Meeting
Local Anesthetic Use in Tumescent Liposuction: An American Society of Plastic Surgeons (ASPS) Survey
Angie M. Paik, B.A.1, Lily N. Daniali, M.D.1, Edward S. Lee, M.D.1, Henry C. Hsia, M.D., FACS2.
1Rutgers University - New Jersey Medical School, Newark, NJ, USA, 2Rutgers University - Robert Wood Johnson Medical School, New Brunswick, NJ, USA.
Background: Current guidelines favor the use of lidocaine as the local anesthetic of choice in liposuction wetting solutions. The use of bupivacaine as an alternative remains controversial despite reports of its use with safe outcomes. The goals of this study were to determine the prevalence of bupivacaine use in wetting solutions, examine the liposuction practices of bupivacaine users, and elucidate opinions regarding bupivacaine use in tumescent liposuction.
Methods: An online survey was distributed to 2,500 randomly-selected members of the American Society of Plastic Surgery. Data was collected and analyzed with emphasis on comparing the liposuction practices and opinions of those who use bupivacaine and those who do not use bupivacaine.
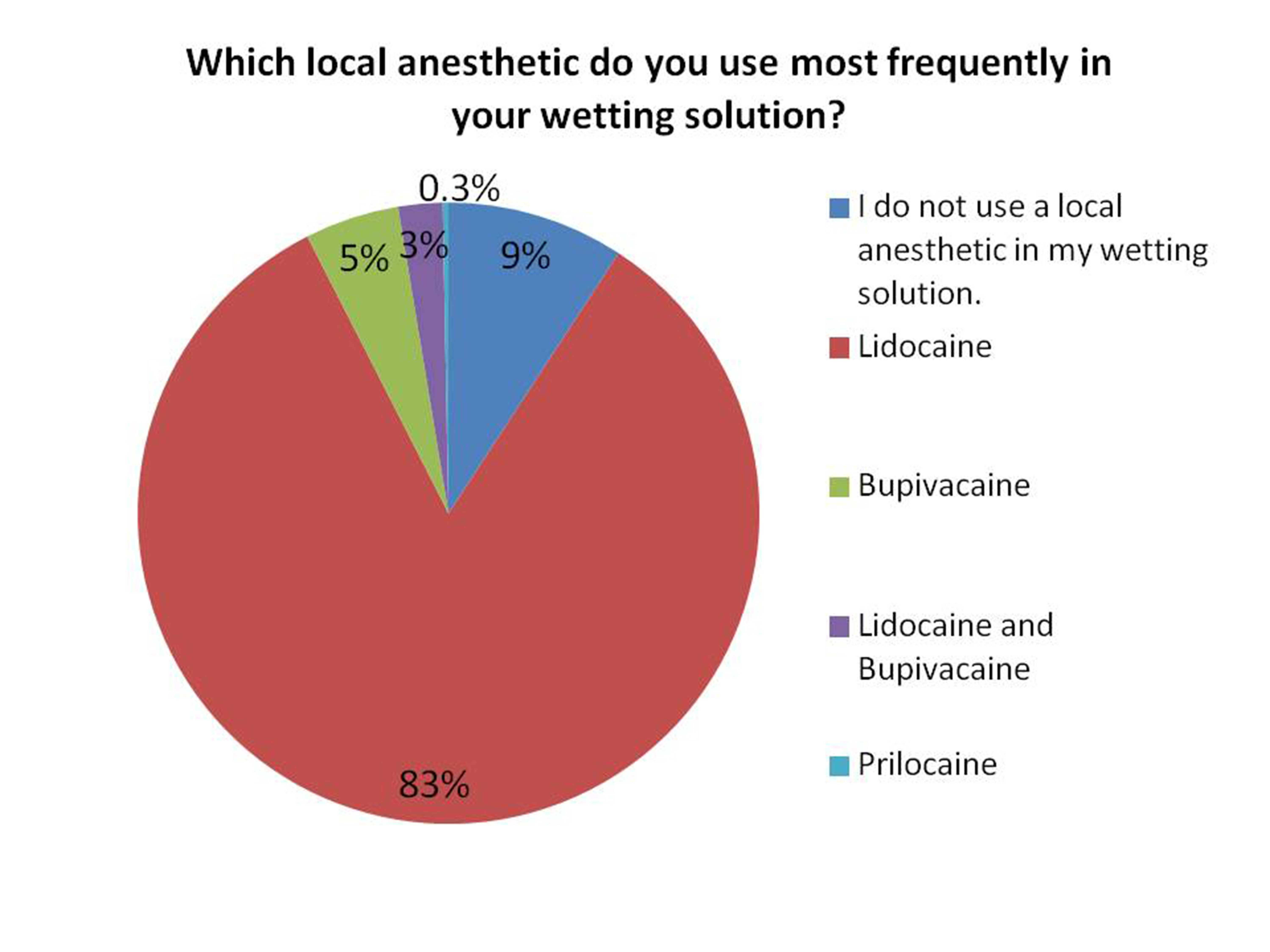
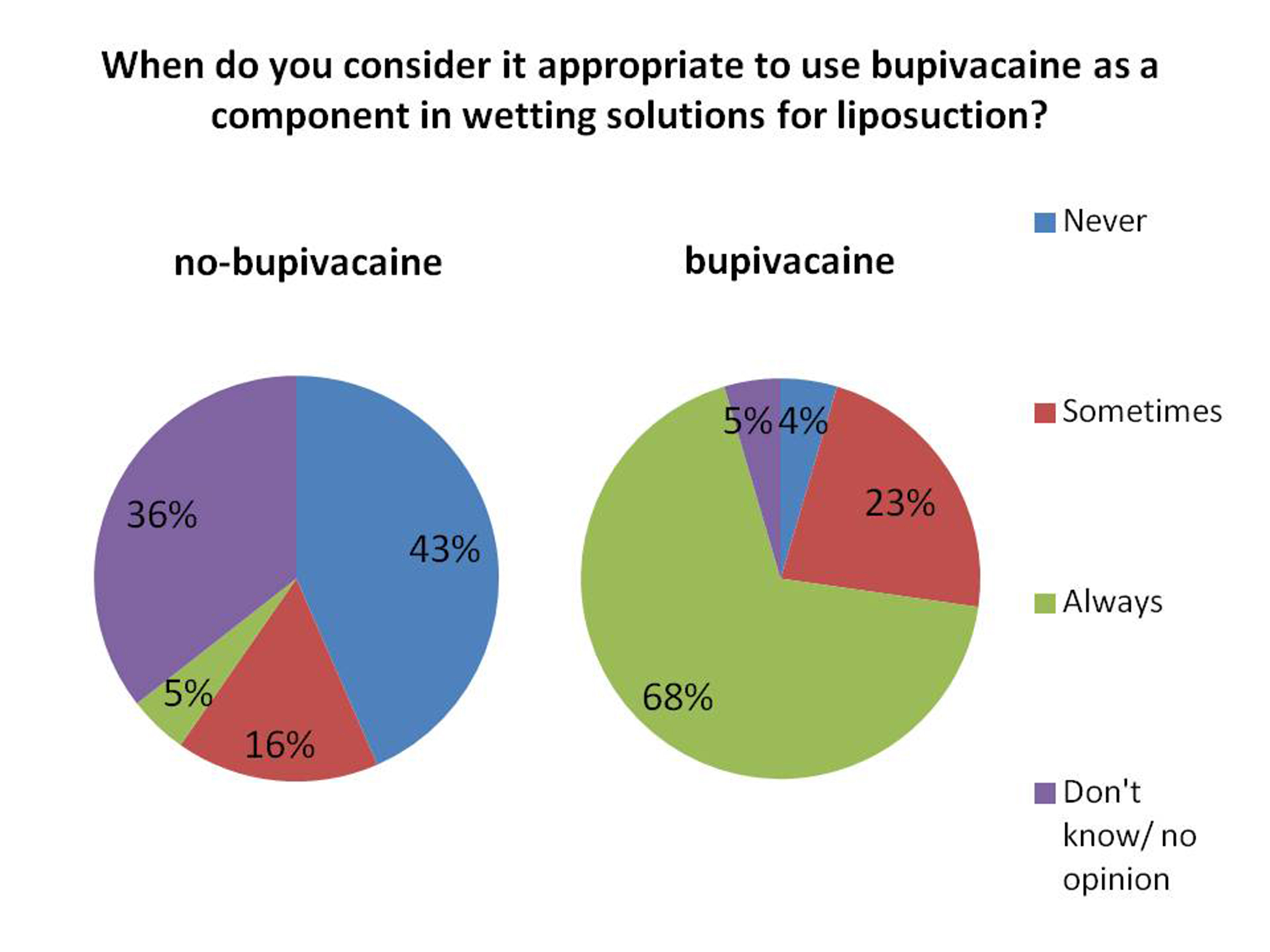
Results: The response rate of the survey was 12.8% (n=320). 7.2% (n=22) of respondents reported using bupivacaine in their wetting solutions (bupivacaine group) (Figure 1). 83.5% (n=254) of respondents reported using either lidocaine or prilocaine (no-bupivacaine group). The demographic profile and liposuction practices of the bupivacaine group were comparable to those of the no-bupivacaine group. Although 36% of the no-bupivacaine group did not know or had no opinion on when it is appropriate to use bupivacaine in liposuction (Figure 2), 85% of this group use bupivacaine in other pain control modalities. There were no reports of bupivacaine toxicity in 2011. The only cases of toxicity reported were associated with lidocaine use in wetting solutions.
Conclusion: A review of 320 plastic surgeons’ experiences revealed that 7% of respondents are using bupivacaine in their liposuction wetting solutions with no reported cases of toxicity. Bupivacaine users differed dramatically only in their opinion regarding the safety of bupivacaine in tumescent liposuction. Our data support the contention that bupivacaine is no more dangerous
than lidocaine when used appropriately. As the field of plastic surgery continues to evolve into an evidence-based field, a rigorous clinical trial documenting the safety and efficacy of bupivacaine in tumescent liposuction with direct comparison to lidocaine would be warranted.
Back to Annual Meeting
|








