|
Back to Annual Meeting
Primary Treatment of Facial Paralysis in the Oncologic Setting in Patients With Proximal Facial Nerve Sacrifice
Erez Dayan, M.D.1, Mark L. Smith, M.D.1, Mark Sultan, M.D.2, William Samson, M.D.2, Joseph H. Dayan, M.D.1.
1Beth Israel Medical Center, New York, NY, USA, 2St. Luke's Roosevelt Medical Center, New York, NY, USA.
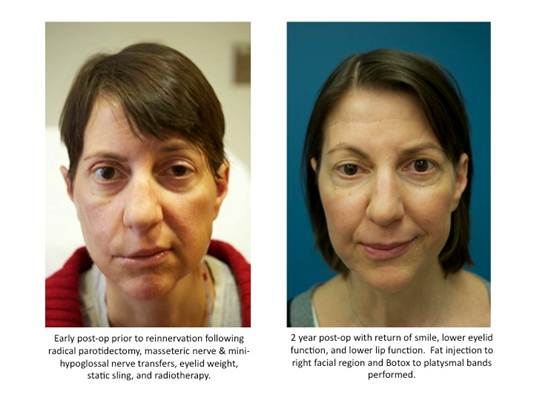
BACKGROUND: Proximal facial nerve sacrifice during tumor extirpation results in complete ipsilateral facial paralysis. Primary nerve grafting requires a long time to reinnervation with variable outcomes and may not be an option if a proximal facial nerve stump is absent. In these cases, patients are often limited to a static sling following completion of adjuvant treatment. If dynamic reconstruction is attempted, rapid and reliable reinnervation is critical in patients with a limited prognosis. This study describes our approach toward primary dynamic restoration of facial nerve function in the oncologic patient using combined nerve-to-masseter and mini-hypoglossal transfers at the time of tumor ablation.
METHODS: A retrospective study was performed on all patients who underwent oncologic resection with proximal facial nerve sacrifice between November 2010 and March 2012. Outcomes evaluated included: Terzis' grading scale, time to reinnervation, speech, oral competence, tongue atrophy, mastication, and post-surgical complications. All patients underwent nerve-to-masseter transfer to the upper division of the facial nerve for smile and lower eyelid tone as well as mini-hypoglossal transfer to the marginal mandibular nerve for lower lip animation at the time of oncologic resection. Primary placement of an eyelid weight was used in all patients, and in isolated cases, a static sling was placed to provide symmetry at rest during the period of reinnervation.
RESULTS: A total of 8 patients were identified. 7 out of 8 patients underwent adjuvant radiotherapy following tumor resection and reconstruction. All patients had evidence of dynamic recovery of smile and lower eyelid function at 3-5 months postoperatively. All patients had oral competence, intelligible speech, no evidence of hemi-tongue atrophy, and no difficulty in mastication or deglutition. All patients had the ability to close the ipsilateral eye with active lower eyelid motion. Because the combined nerve transfers had separate targets, synkinesis was minimal. One patient had a salivary leak related to her parotidectomy that healed spontaneously. There were no other surgical complications.
CONCLUSIONS: The combined use of targeted nerve to masseter and mini-hypoglossal nerve transfers provides rapid and reliable dynamic facial reanimation in patients with locally advanced tumors requiring proximal facial nerve sacrifice. Static procedures may be performed at the same setting to provide symmetry at rest during the 3 -5 month reinnervation period.

Back to Annual Meeting
|








