|
Back to Annual Meeting
An effective method to access recipient vessels outside the zone of injury during free flap reconstruction of lower extremity defects
Emily M. Clarke-Pearson, MD, Daniel Kim, BS, Peter S. Kim, MD.
Beth Israel-Deaconess Medical Center, Boston, MA, USA.
Introduction
A principle of microvascular surgery for lower extremity reconstruction is to identify recipient vessels and perform the anastomosis outside the zone of injury. This zone of injury, described by Godina in his sentinel paper in 1986, is characterized by tissue edema and fibrosis, often the sequelae of chronic inflammation, infection, or radiation therapy. Microsurgeons will often create an incision that extends from the proximal wound several centimeters cephalad to access the recipient vessels outside the zone of injury. This iatrogenic wound, however, traverses the zone of injury, and is susceptible to delayed healing and wound breakdown, particularly at the T-junction. These complications can be avoided by creating a unique incision proximal to the zone of injury through which the recipient vessels are dissected and the anastomosis performed. We present a series of patients treated with this surgical technique and their results.
Methods
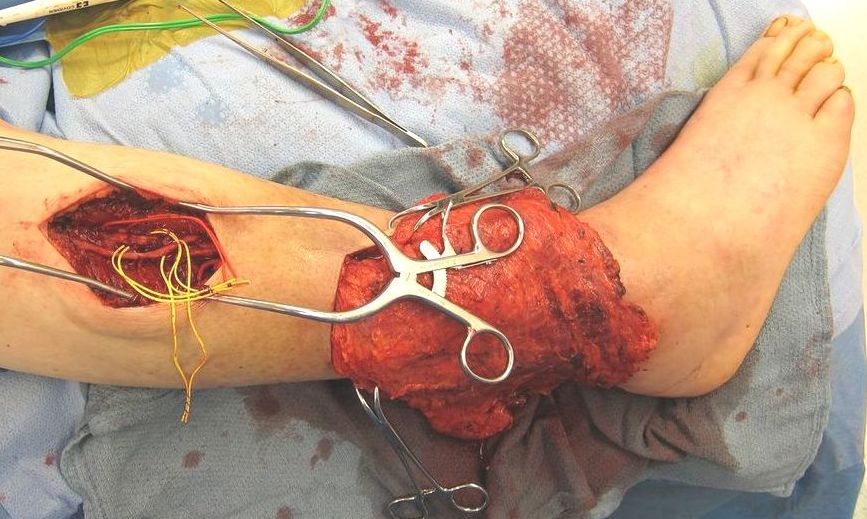
Thirteen consecutive patients from 2011-2013 underwent free flap closure of a lower extremity defect using the following approach: An incision was made proximal to the lower extremity defect to avoid incising from the edge of the defect through damaged tissue. Clinical exam was used to determine where healthy tissue resumed outside the zone of injury. The pedicle was gently tunneled in the subcutaneous plane from the defect to reach the recipient vessels, with care taken before tunneling to ensure hemostasis both within the tunnel and of the pedicle. Hand-sewn arterial anastomoses were performed, and 1 to 3 veins were coapted with either couplers or suture in each patient. The remote incision was closed in layers and the flap inset. Drains were used infrequently. Figures 1-2.
Results
Three female and ten male patients were included. Median age was 65 years (18-85). Etiology of the wounds was trauma (3 acute, 7 chronic), oncologic (2), and ischemic (1). Defects varied in size from 6-30 cm long and 4-15 cm wide, and were primarily located on the distal third of the extremity. Free flaps included radial forearm (4), ALT (4), gracilis (2), vastus (1), latissimus dorsi (1), and parascapular (1). Drains were used in 4 patients only. Postoperatively, there were no major complications related to the flaps or any flap losses. There was one donor site hematoma requiring operative evacuation. There were no complications associated with the anastomotic incision.
Conclusions
Accessing the recipient vessels via a separate proximal incision in lower extremity free flap reconstruction allows excellent exposure outside the zone of injury, and avoids extending the wound and creating a vulnerable T-junction. When tunneled in the subcutaneous plane, there is low risk of pedicle compression. Additionally, the pedicle does not coil within the defect, and is in a safer position if reoperation for orthopedic fixation or flap debulking is required.

Back to Annual Meeting
|







