|
|
 |
Back to Annual Meeting
Population Preferences of Undergoing Brachioplasty for Arm Laxity
Ahmed M. S. Ibrahim, M.D.1, Hani H. Sinno, M.D., MEng2, Ali Izadpanah, M.D., MSc2, Joshua Vorstenbosch, PhD2, Tasso Dionisopoulos, M.D.2, Bernard T. Lee, MD, MBA1, Samuel J. Lin, M.D1
1Harvard Medical School/Beth Israel Deaconess Medical Center, Boston, MA, USA, 2McGill University, Montreal, QC, Canada.
BACKGROUND:
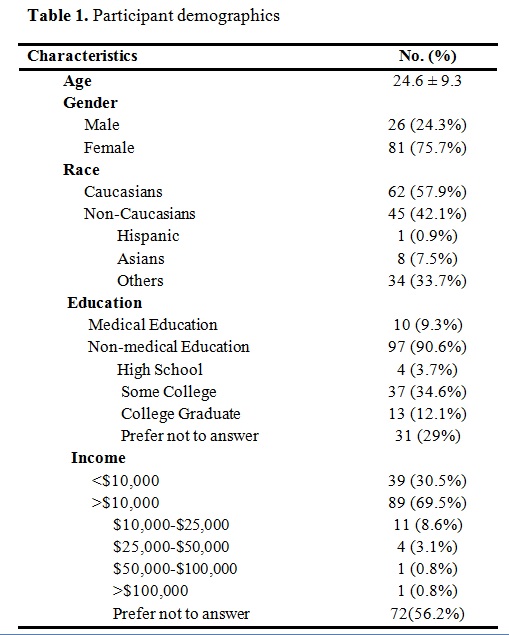
Contour changes of the upper arm can occur with increasing age or following massive weight loss to which surgical procedures can address the degree of deformity. The number of patients requesting surgical procedures performed for brachioplasty and massive weight loss is increasing. In order to gain a better understanding of the health burden associated with living with an arm deformity requiring brachioplasty, we aimed to objectify this health state with validated measures.
METHODS:
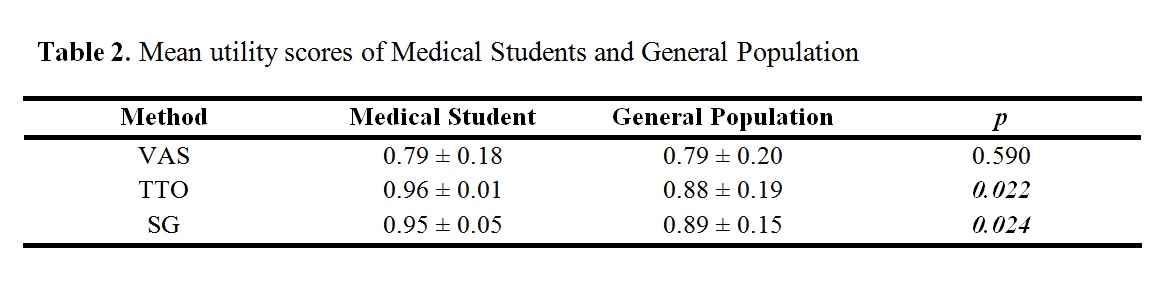
Utility assessments using the visual analog scale (VAS), time trade-off (TTO), and standard gamble (SG) were used to obtain utilities scores for arm deformity, monocular blindness, and binocular blindness from a sample of the general population and medical students. Linear regression and student t-test were used for statistical analysis. A p<0.05 was deemed statistically significant.
RESULTS:
All the measures for arm deformity of the 107 volunteers (VAS, 0.80 ± 0.14; TTO, 0.91 ± 0.12; SG, 0.94 ± 0.10) were significantly different (p < 0.001) from the corresponding measures for monocular blindness (0.65 ± 0.16, 0.87 ± 0.14, and 0.87 ± 0.14, respectively) and binocular blindness (0.36 ± 0.18, 0.67 ± 0.25, and 0.69 ± 0.2, respectively). When compared to the sample of the general population, having a medical education demonstrated a statistical significance of being less likely to trade years of life and less likely to gamble risk of mortality for a procedure such as a brachioplasty. Race and sex were not statistically significant independent predictors of risk acceptance.
CONCLUSIONS:
We have objectified the health state of living with upper arm deformity requiring brachioplasty. Utility outcome scores were comparable to living with health states such as aging neck needing rejuvenation and massive weight loss requiring panniculectomy.
Back to Annual Meeting
|








