|
Back to Annual Meeting
Alloderm Reduces Capsule Formation in Two-Stage Breast Reconstruction Following Mastectomy
Jamil A. Matthews, MD, Jennifer Sabino, MD, Alexandra Conde-Green, MD, Devinder Singh, MD.
University of Maryland Medical Center, Baltimore, MD, USA.
Background: Breast reconstruction with tissue expansion and implant placement is a main treatment modality following mastectomy for breast cancer. The use of acellular dermal matrix to create an inferior pocket for the tissue expander or implant is becoming more prevalent with multiple studies reporting positive results. However, capsular contracture remains a significant complication, causing pain, deformity, dissatisfaction, and often the need for reoperation for contracture release or excision. We sought to determine whether the use of acellular dermal matrix, placed at the first stage of reconstruction, decreases the amount of capsule formation at implant exchange. We hypothesize that the area of the pocket in contact with the Alloderm will have less scar than the that in contract with the native pectoralis muscle.
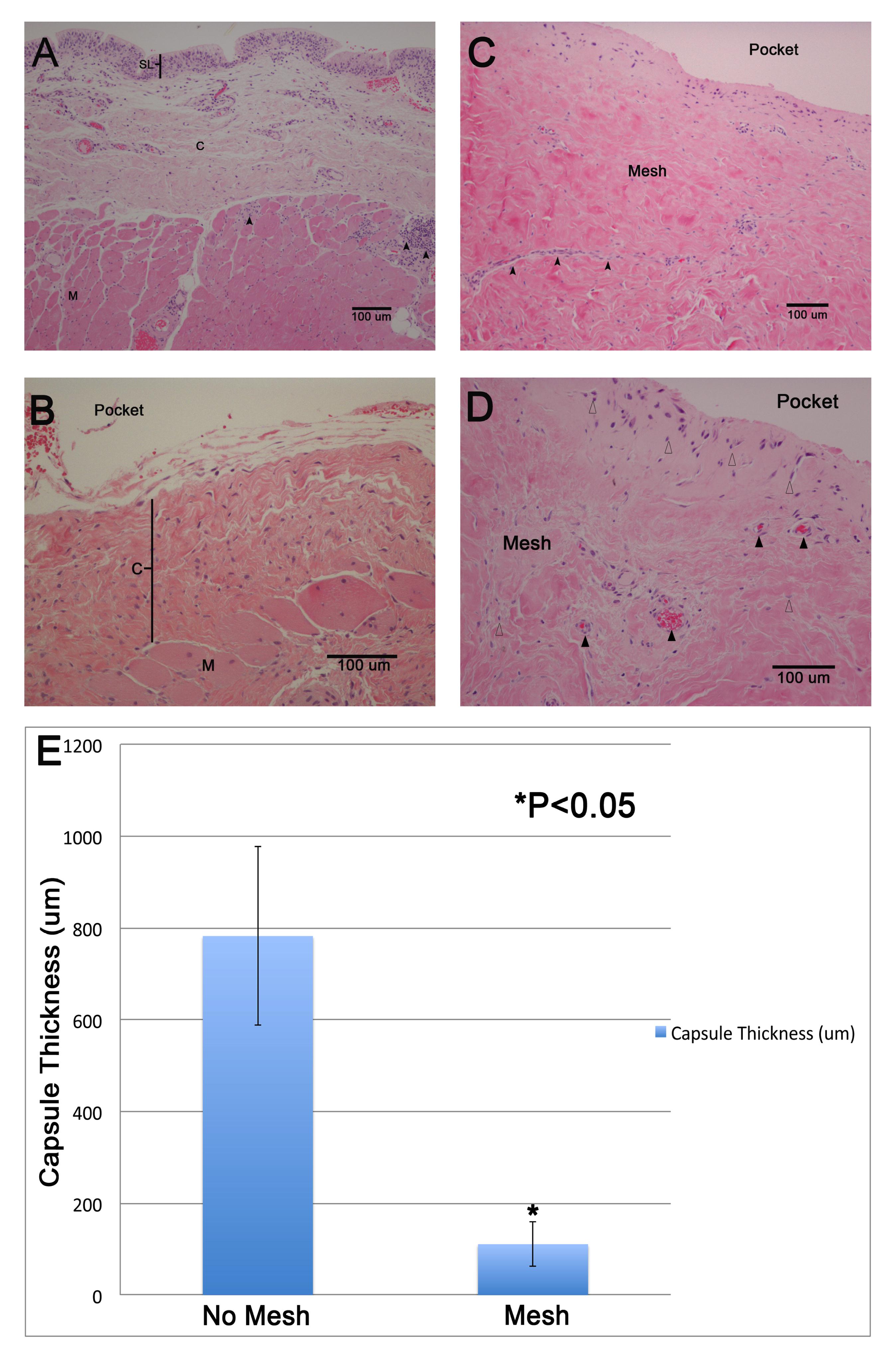
Methods: Patients (10) who underwent a unilateral or bilateral mastectomy as part of their breast cancer treatment and had their two-stage reconstruction with Alloderm and implants were included in this study. At the time of exchange of the breast tissue expander, a small biopsy was obtained from the capsule and the posterior pectoralis muscle adjacent to the pocket. Paraffin embedded, formalin fixed sections of the excised tissue was stained for hematoxylin and eosin for histology. Immunohistochemical analysis was performed with smooth muscle actin (alpha-SMA), a marker for myofibroblasts commonly seen in scar and VVG, a marker for collagen. Capsular thickness, as determined by histology was measured using photoshop software, standardized to scale under identical magnification.
Results: Capsule thickness was significantly greater in the areas of tissue in direct contact with the tissue expander (782 +/- 194 um) compared to those covered with Alloderm (47.91 +/- 110.82 um; P<0.05). In fact, the component of scar within the mesh contained only a layer of pseudostratified columnar epithelium (synovial layer) which lack the myofibroblasts that are implicated in scar contracture. Analysis of the capsule demonstrated infiltration of neutrophils, diffuse deposition of collagen and myofibroblast infiltration. Positive SMA staining was seen throughout the capsule confirming the presence contractile smooth muscle cells (not shown). Fibroblast infiltration and blood vessel formation is seen in the mesh at the time of biopsy.
Conclusion: Alloderm, when placed in the pocket at the first stage of reconstruction, significantly reduces breast capsule formation in comparison to the patient’s native tissues. This can reduce patient pain, dissatisfaction, morbidity and surgical costs. The study can serve to modify current techniques in breast reconstruction.
Back to Annual Meeting
|







