Back to 2015 Annual Meeting
Implant-Based Breast Reconstruction with Pectoralis-Serratus Sling and Acellular Dermal Matrix
Adam R. Kolker, M.D., Paulo Piccolo, M.D..
Icahn School of Medicine at Mount Sinai, New York, NY, USA.
Background: Partial muscle coverage with the use of acellular dermal matrices (ADM) has become widely integrated in implant-based breast reconstruction. The advantages have included greater primary implant fill volumes and improved breast aesthetics compared with total muscle coverage. In this study, we evaluate a technique of increased muscle coverage combined with ADM that maintains the lateral integrity of the pectoralis major muscle in continuity with the serratus anterior muscle.
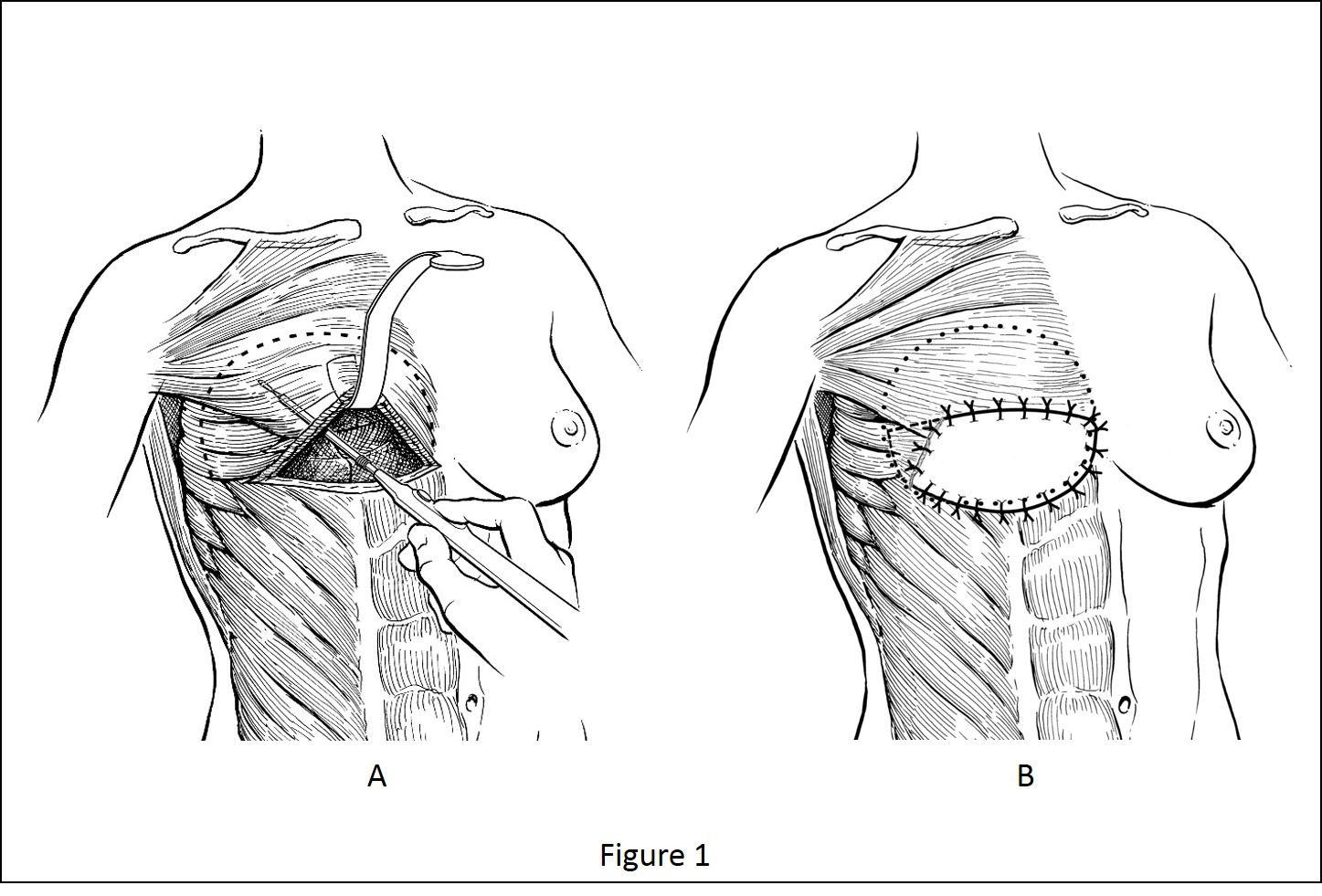
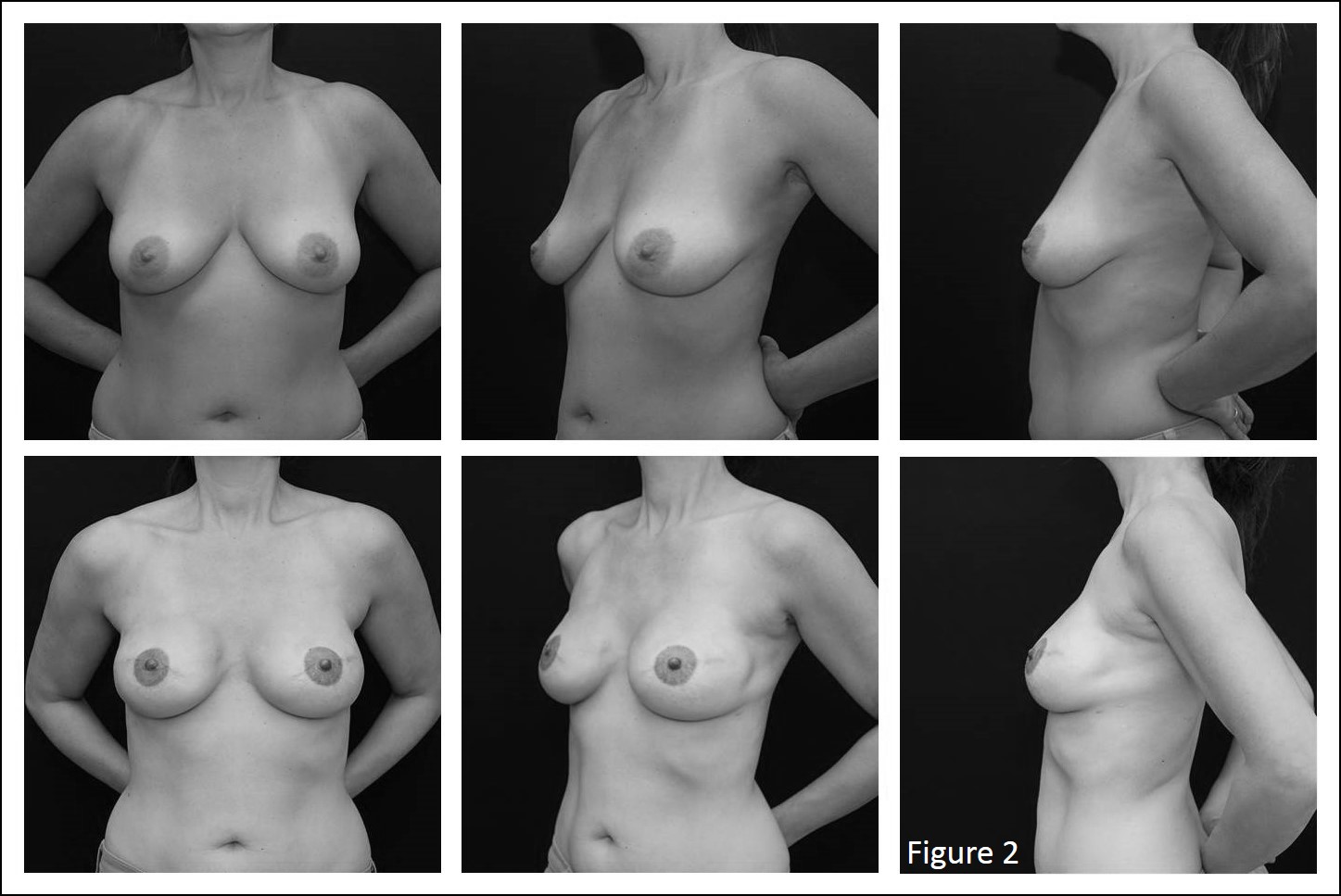
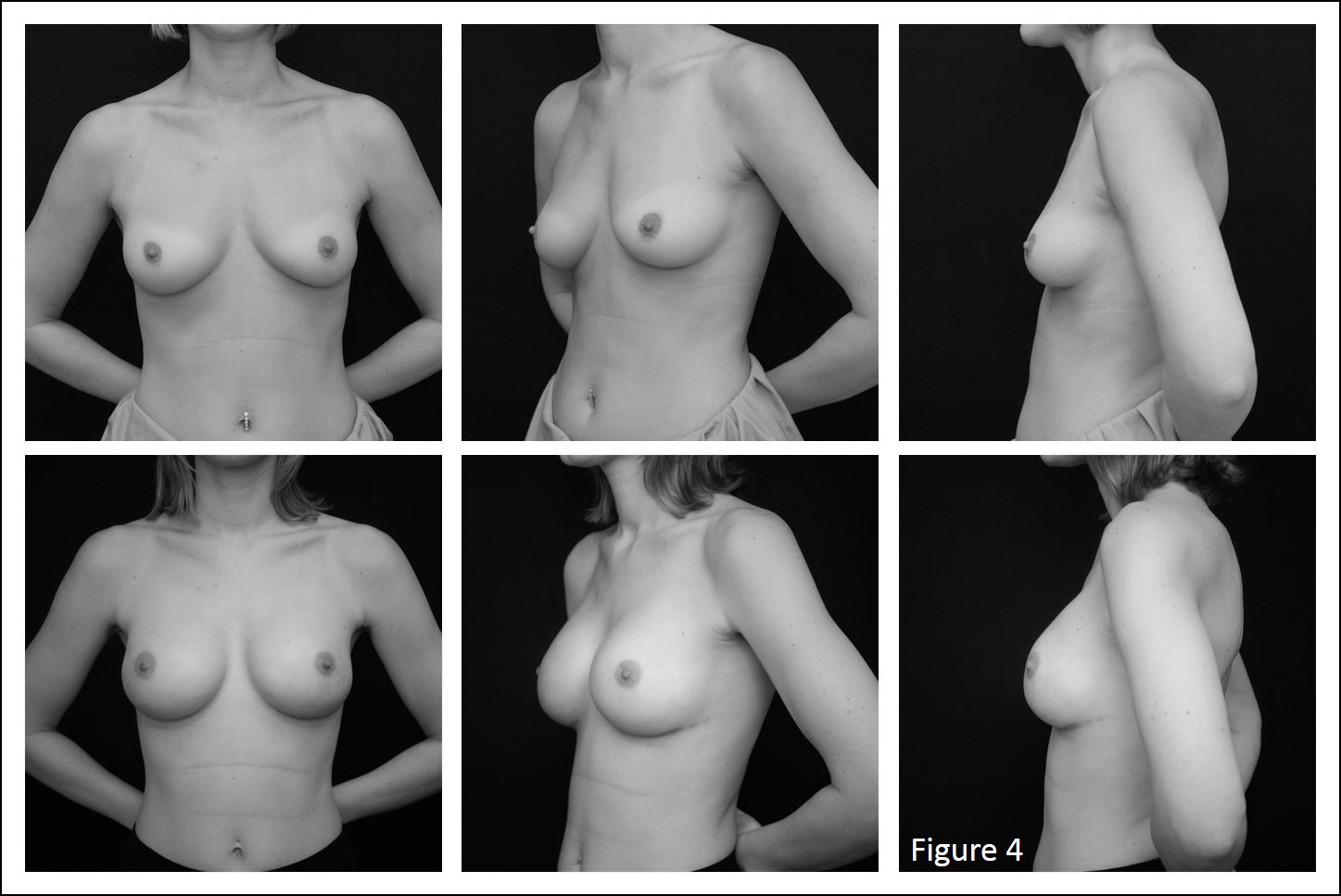
Methods: A retrospective review of patients treated over 36 months was performed. Surgical technique involves horizontal division of the inferior pectoralis major origins followed by retropectoral pocket dissection; at the lateral border of the pectoralis minor, dissection is carried deep to the serratus anterior muscle maintaining a continuous lateral sling with the pectoralis major (Figure 1a). ADM is then affixed to the incised caudal margin of pectoralis major, the prosthesis is inserted into the pocket, and the ADM affixed inferiorly and tucked beneath serratus muscle laterally (Figure 1b). The surgical technique and aesthetic results are presented (Figures 2-4). Outcome parameters included postoperative complications, rates of revision, and postoperative Breast-Q satisfaction scores.
Results: The study sample was comprised of 140 reconstructed breasts in 82 patients with mean follow up of 17 months. There were 58 women who underwent bilateral reconstruction, and 24 unilateral. All cases were two-stage reconstructions with primary tissue expander insertion. There were 18 prophylactic mastectomies (36 breasts), and 14 nipple sparing mastectomies (28 breasts). Nineteen (19 breasts) received radiation therapy (RT) postoperatively. Infections were treated successfully in 7 (4%), 3 with antibiotics only, and 4 with reoperation (washout and prosthetic exchange). There was 1 hematoma, 2 seromas, 5 minor necroses, and 1 major necrosis. Nine patients (11%) required unplanned revision, 4 of which followed RT. Breast-Q postoperative mean scores were: satisfaction with outcome 78 ± 10, satisfaction with breasts 71 ± 9, psychosocial well-being 75 ± 12 and sexual well-being 60 ± 17.
Conclusions: The maintenance of continuity between the pectoralis major and serratus anterior muscles in prosthetic breast reconstruction with ADM provides thicker inferolateral and lateral vascularized autogenous implant coverage and establishes improved support and maintenance of implant position. With the aesthetic benefits, acceptable complication profile, low revision rate, and high patient quality of life and satisfaction outcomes, this surgical approach should be considered for implant based breast reconstruction.
Back to 2015 Annual Meeting
|




