Back to 2015 Annual Meeting
Open Surgical Training Model for Breast Reconstruction
John T. Stranix, MD, Jennifer Thompson, BS, Alexes Hazen, MD.
New York University, New York, NY, USA.
BACKGROUND: According to the American Society of Plastic Surgeons' annual report, over 445,000 cosmetic and more than 176,000 reconstructive breast procedures were performed by ASPS member surgeons in 2013. These numbers continue to increase each year, and reinforce the need for plastic surgery training programs to produce graduates with both a comprehensive understanding of breast surgery and the technical skills required to reconstruct a wide variety of acquired breast defects. Multiple randomized controlled trials and systematic reviews have demonstrated the effectiveness of simulator-based surgical education; however, there has been a lack of its incorporation into plastic surgery training. Currently, no high-fidelity model exists for open surgical training of breast reconstruction. The purpose of this project was to develop a surgical training model that accurately replicates female breast anatomy and provides a useful tool to supplement and standardize plastic surgery resident education.
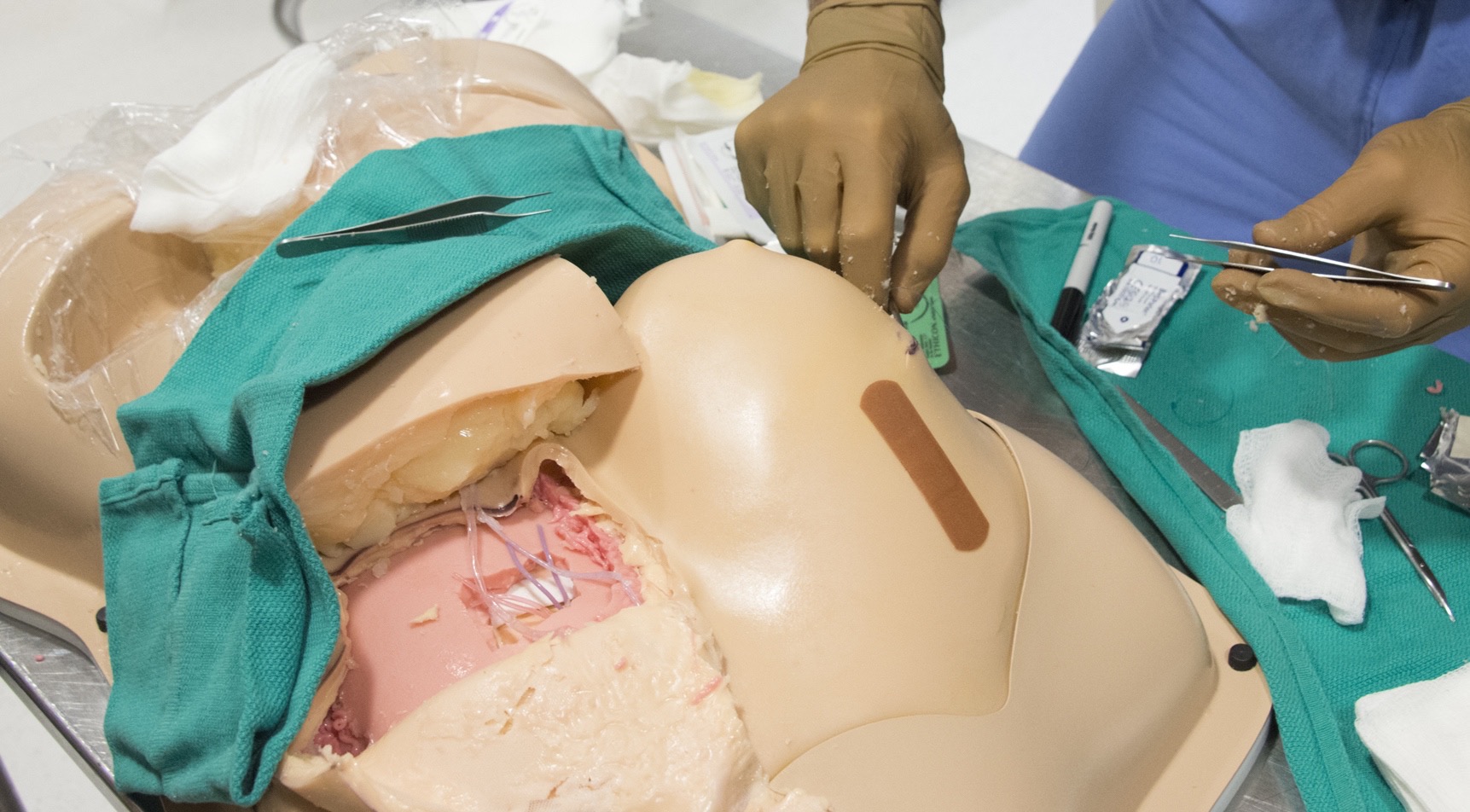
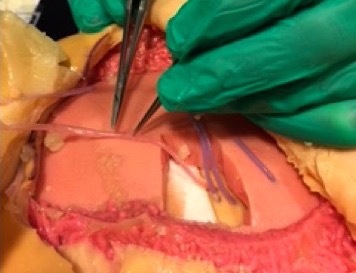
METHODS: In conjunction with The Chamberlain Group medical modeling company, a scale model of the female chest and abdomen was constructed using artificial materials designed to reproduce the appearance and feel of living human tissue. Epidermis, dermis, subcutaneous fat, breast glandular tissue, muscle, cartilage, bone, and perforating arteries and veins were all represented. Upon completion of the initial prototype, plastic surgery residents and attendings used the model to perform local tissue rearrangements including nipple reconstruction, lumpectomy, mastectomy, and abdominal free flap reconstruction with microvascular anastomoses to internal mammary perforators. Throughout these procedures, surgeons' feedback regarding modifications necessary to make the model more closely approximate human tissue was recorded. These modifications were then incorporated into the subsequent prototype and the process repeated until the model accurately replicated the anatomic planes and tactile feedback of a living breast.
RESULTS: Working closely with a medical modeling company, we were able to design an open surgical training model of the female breast capable of simulating procedures ranging from local tissue rearrangement to mastectomy with free flap reconstruction. To our knowledge, this model represents the first of its kind in plastic surgery.
CONCLUSIONS: A high-fidelity surgical model of female breast reconstruction has potential to serve as a useful tool to supplement plastic surgery resident training. As more plastic surgery residency programs become fully integrated, this realistic simulator may prove particularly valuable for teaching surgical techniques to junior residents. Validation of this simulator and its incorporation into a comprehensive breast surgery curriculum for plastic surgery residents is currently underway.
Back to 2015 Annual Meeting
|




