|
|
|
|
|
Back to 2015 Annual Meeting
Cost-effectiveness Analysis Of Breast Reconstruction Options In The Setting Of Postmastectomy Radiotherapy Using The BREAST-Q.
Shantanu N. Razdan, MD, MSPH, Peter G. Cordeiro, MD, Claudia R. Albornoz, MD, MSc, Teresa Ro, BS, Wess A. Cohen, MD, Babak J. Mehrara, MD, Joseph H. Dayan, MD, Colleen M. McCarthy, MD, MS, Joseph J. Disa, MD, Andrea L. Pusic, MD, Evan Matros, MD, MMSc.
Memorial Sloan Kettering Cancer Center, New York, NY, USA.
Background: There is no consensus on a uniform reconstructive algorithm for patients with locally advanced breast cancer who require PMRT. Both delayed autologous and immediate prosthetic techniques have inherent advantages and complications. The study hypothesis is that implants are more cost-effective than autologous reconstruction in the setting of PMRT because of immediate restoration of the breast mound. Such information can be used to rationalize reconstructive decision making in a resource constrained healthcare environment.
Methods: A cost-effectiveness analysis model using the payer perspective was created comparing delayed autologous and immediate prosthetic techniques against the do-nothing option (i.e. mastectomy without reconstruction). The base case analysis assumed a life expectancy of 7 years for the average patient with breast cancer requiring PMRT. A decision tree was created that included possible complications with associated probabilities. Costs were obtained from Nationwide Inpatient Sample 2010 database. Effectiveness was determined using the Breast-Q patient reported outcome measure. A Breast-QALY was considered one year of perfect breast health related quality of life. Incremental cost-effectiveness ratio (ICER) was calculated for both treatment options compared to the do-nothing option. Willingness-to-pay (WTP) threshold was set at \,000. One-way sensitivity analysis was performed by varying the life expectancy.
Results: Breast-Q scores were obtained from patients who underwent immediate prosthetic reconstruction (n=196), delayed autologous reconstruction (n=76) and mastectomy alone (n=71). Breast-QALYs were greatest for autologous followed by implant and no reconstruction. Costs were lowest for no reconstruction, followed by implants, and autologous transfer (Table 1). The ICER for immediate prosthetic and delayed autologous reconstruction compared to mastectomy alone was \,906 and \,509 respectively. Sensitivity analysis showed that the ICER for both treatment options decreased with increasing life expectancy (Figure 1).
Conclusion: Immediate prosthetic based breast reconstruction is a cost-effective approach for women who require PMRT. If greater life expectancy is anticipated, autologous transfer becomes cost-effective as well and may be a superior option due to higher Breast-Q scores associated with this method in the long-term.
Results of a base case cost-effectiveness analysis.| Treatment | Cost (\0 | Incremental Cost (\0 | Effect (Breast-QALY) | Incremental Effect (Breast-QALY) | ICER (\
Breast-QALY) | | Mastectomy without Reconstruction | 23,297 | - | 4.03 | - | - | | Immediate TE/Implant Reconstruction | 61,515 | 38,218 | 4.69 | 0.66 | 57,906 | | Delayed Autologous Reconstruction | 101,204 | 77,907 | 4.79 | 0.76 | 102,509 | 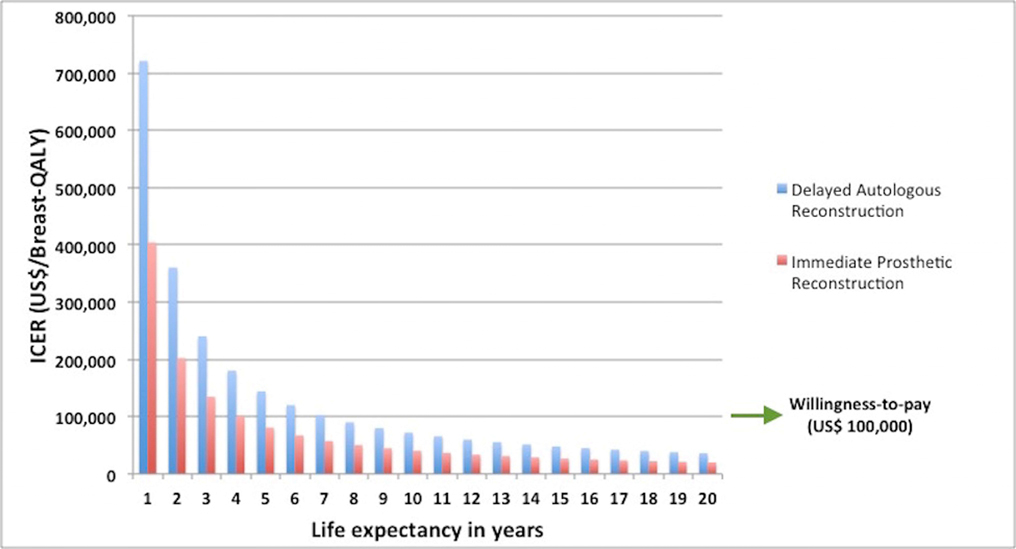
Back to 2015 Annual Meeting
|
|




