Back to 2015 Annual Meeting
Dental Rehabilitation in More Complex Mandibular Reconstructions using Free Fibula Flaps: The Power of Virtual Surgical Planning
Casian Monaco1, Tomer Avraham2, John T. Stranix1, Lawrence Brecht1, David L. Hirsch1, Jamie P. Levine1.
1NYU Langone Medical Center, New York, NY, USA; 2Mount Sinai Health System and Icahn School of Medicine, Department of Surgery, Division of Plastic Surgery, New York, NY,USA.
BACKGROUND:
Virtual surgical planning (VSP) and its use in mandible reconstruction has been well described. Our group has used it to implement a number of technical refinements that are unique. Today, we routinely perform complex reconstructions that involve several of these. Primary endosteal implants with dental prostheses, double barreling techniques, custom reconstruction bars and aesthetic-based orthognathics are now tools routinely implemented because of this technology. This study intends to investigate the trends of mandible reconstruction at our institution with a particular focus on dental rehabilitation.
METHODS:
We performed a retrospective chart review on all patients who underwent VSP-assisted mandible reconstruction with free fibula flaps at our institution's university and county-affiliated hospitals. Patient, disease, and procedure specific variables were recorded and analyzed. Results from key eras were compared and analyzed.
RESULTS:
Between October 2008 and February 2015, 76 patients underwent a total of 78 VSP-assisted mandible reconstructions with free fibula flaps. Twenty four flaps had implants primarily placed (30.8%) and seven of these had immediate placement of a dental prosthesis as well. Twenty five flaps (32.1%) included a double-barrel segment to allow for greater construct height. Of these, eight flaps (10.3%) had a wedged double barrel component if it was located laterally.
The cohort was divided into three distinct eras. The first generation involved the initial cases using VSP technology from October 2008 to January 2010. These 12 flaps simply spanned the bony defects and any implant placement was estimated intra-operatively. The second generation describes flaps reconstructed from February 2010 to January 2014. February 2010 was the first time implant placement was digitally simulated with the reconstruction pre-operatively. The third generation spans from January 2014 to the most recent case performed in February 2015. These 11 flaps are all of the flaps performed since reconstruction bars were digitally pre-planned and directly milled pre-operatively in January 2014.
Overall, 47 patients (60.3%) achieved dental implant placement with 35 (45%) going on to full dental rehabilitation with implant based, fixed prosthesis. 62 % of patients were able to tolerate a solid diet postoperatively. The only significant difference amongst the groups was in number of implants (p = 0.017). There was a trend toward increasing percentage of patients receiving full dental rehabilitation with fixed prosthesis. This complete dental rehab occurred in the setting of increased number of innovations per flap (p < 0.001). Dental Rehabilitation by Era | Total | | First Generation | | Second Generation | | Third Generation | | p-value | | Dental Implants (n, %) | 47 | 60% | 6 | 50% | 32 | 58% | 9 | 82% | 0.251 | | Immediate Dental Implants (n, %) | 24 | 31% | 3 | 25% | 15 | 27% | 6 | 55% | 0.181 | | Number of Implants (mean, SD) | 4.1 | ±1.6 | 3.8 | ± 1.7 | 4.6 | ± 1.4 | 2.7 | ± 1.6 | 0.017 | | Fixed Prosthesis (n, %) | 35 | 45.0% | 4 | 33% | 24 | 44% | 7 | 64% | 0.325 | | Solid Diet Tolerated (n, %) | 45 | 62% | 8 | 67% | 29 | 53% | 8 | 73% | 0.373 | | Innovations per flap (mean, SD) | 1.6 | ± 1.6 | 0.83 | ± 0.94 | 1.4 | ± 1.3 | 3.6 | ± 2.2 | p < 0.001 | CONCLUSIONS:This report demonstrates that virtual planning and computer aided manufacturing have permitted more complex reconstructions with refined innovations while maintaining dental rehabilitation rates. Virtual surgical planning has revolutionized this complex surgery and ushered in the next generation of mandible reconstruction 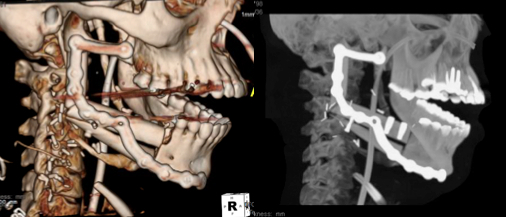
Back to 2015 Annual Meeting
|




