|
|
|
|
|
Back to 2015 Annual Meeting
Insights from the Largest International Experience with Autologous Reconstruction in Nipple-Sparing Mastectomy
Michael Alperovich, MD1, Jordan D. Frey, MD1, Robert J. Allen, Jr., MD1, Neil Tanna, MD2, Jamie P. Levine, MD1, Pierre B. Saadeh, MD1, Mihye Choi, MD1, Nolan S. Karp, MD1, Christina Y. Ahn, MD1, Robert J. Allen, Sr., MD1.
1NYU Langone Medical Center, New York, NY, USA, 2North Shore-Long Island Jewish Medical Center, New Hyde Park, NY, USA.
BACKGROUND:
Implant-based reconstruction has been favored for nipple-sparing mastectomy (NSM) due to the lower BMIs of this patient population and surgeon preference. We reviewed our institutional experience with autologous reconstruction following NSM.
METHODS:
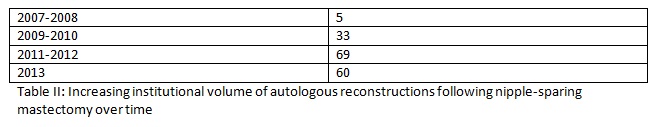
Records of all patients who underwent NSM and autologous reconstruction from 2007-2013 were reviewed.
RESULTS:
Autologous reconstruction was used for 167 NSM in 108 patients. Mean patient age and BMI were 47.6 and 25.8, respectively. Mastectomy indications included both therapeutic (35.9%) and prophylactic (64.1%).
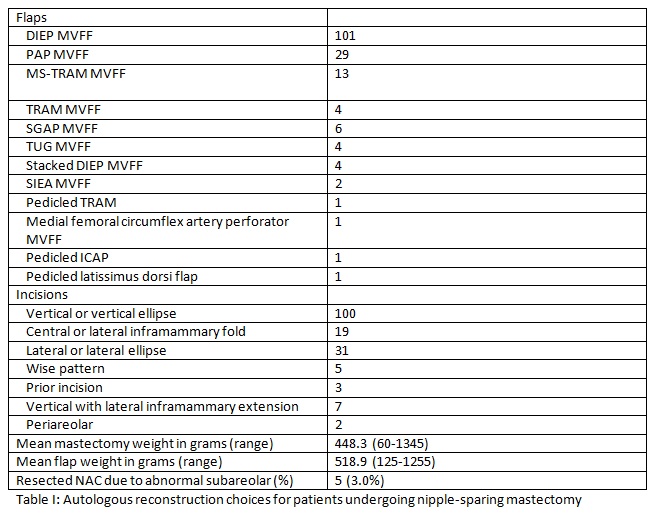
Over 1/4 of flap reconstructions (25.1% of 42/167) were from non-abdominal donor sites. Table I summarizes the distribution of flap and incision choices. The DIEP was the most common flap used (101), and most common access was vertical incision or ellipse (100). Mean mastectomy weight was 448.3 grams (60-1345 grams), and mean flap weight was 518.9 grams (125-1255 grams).
Flap complications included 1 arterial thrombosis (0.6%) and 4 venous thromboses (2.4%). All flaps remained viable except for 1 partial (0.6%) and 1 complete (0.6%) flap loss.
CONCLUSIONS:
We present the largest international experience with autologous reconstruction for NSM. Given the more limited abdominal donor sites in this relatively lower BMI population, comfort with more variable autologous reconstruction techniques is necessary.
Back to 2015 Annual Meeting
|
|




