Back to 2015 Annual Meeting
The Diagonal Upper Gracilis (DUG) Flap: A Low Morbidity Alternative to the TUG, GAP, and PAP Flaps
Erez Dayan, M.D.1, Mark L. Smith, M.D.1, Joseph H. Dayan, M.D.2.
1Beth Israel Medical Center, New York, NY, USA, 2Memorial Sloan Kettering Cancer Center, New York, NY, USA.
Background: While the abdominal donor site is often the first choice for autologous breast reconstruction, it may not be an option in some patients. The TUG, GAP, and PAP flaps have been successfully used as alternative donors sites but each has its own limitations in terms of scar location, donor site cosmesis, morbidity, and technical difficulty. Wound healing complication rates as high as 59% have been reported in patients following TUG flap harvest. In this study, we present a modified gracilis flap design oriented parallel to Langer's lines which allows for greater flap volume and reduced donor site morbidity. The purpose of this study is to assess our four-year experience with this technique.
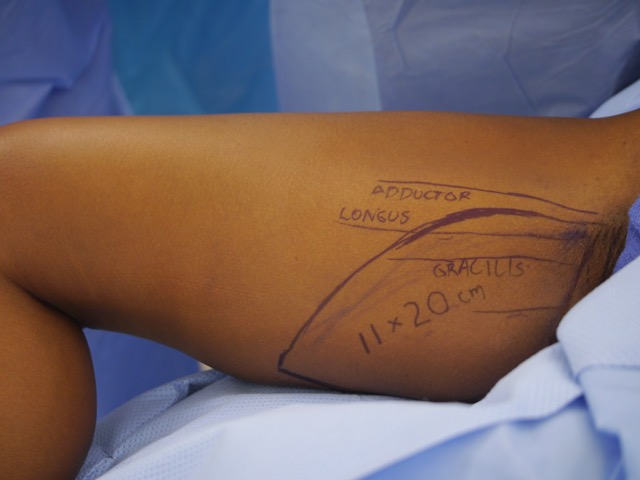
Methods: Prospectively collected data from April 2011 to March 2015 was analyzed for flap volume, dimension, indication, and complications. Flap design: the superior apex of the flap is marked at the adductor longus prominence in the groin crease. The axis of this flap is then marked oblique and posterior, parallel to Langer's lines where a pinch test determines the flap width (Figure 1).
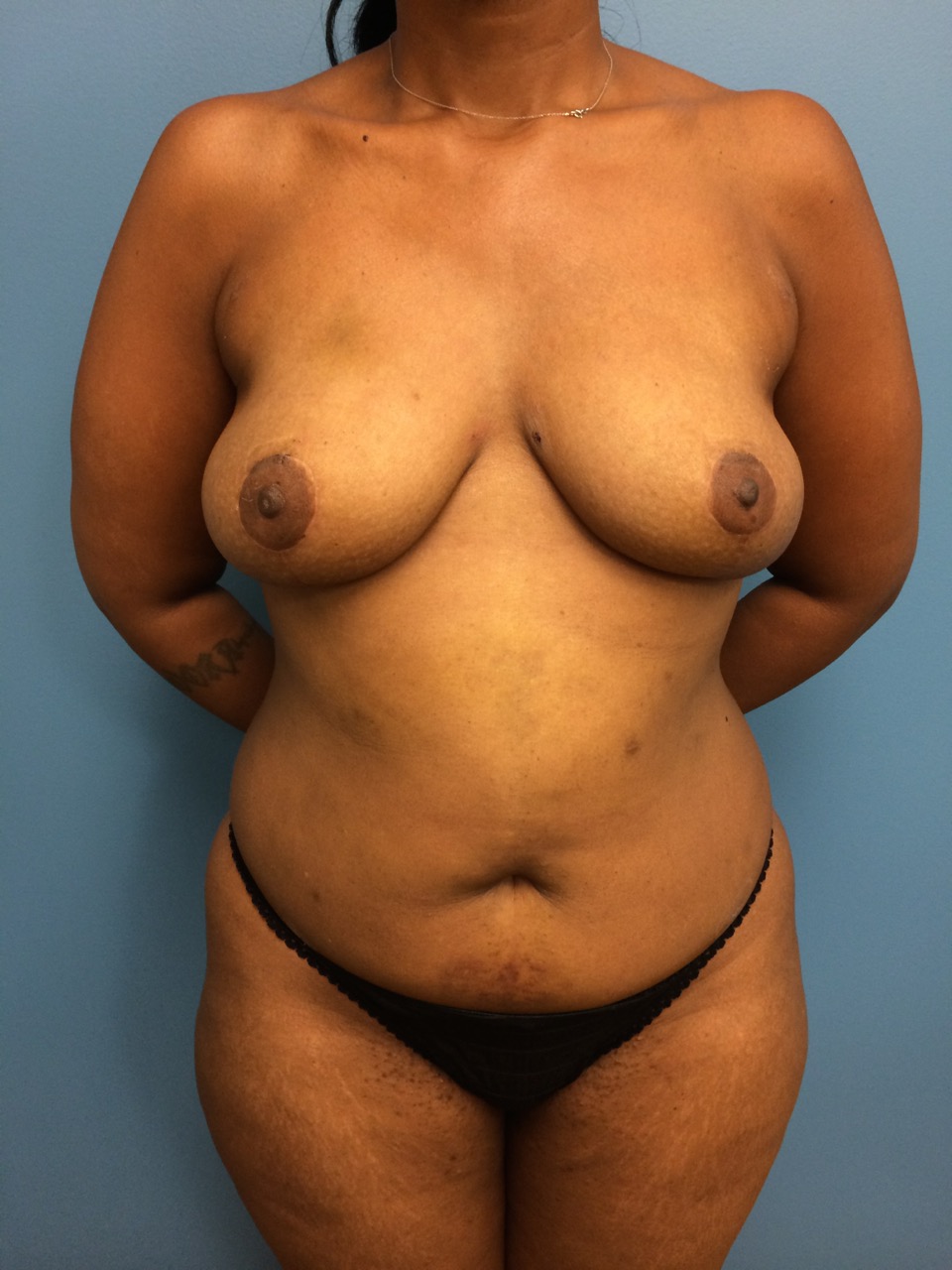
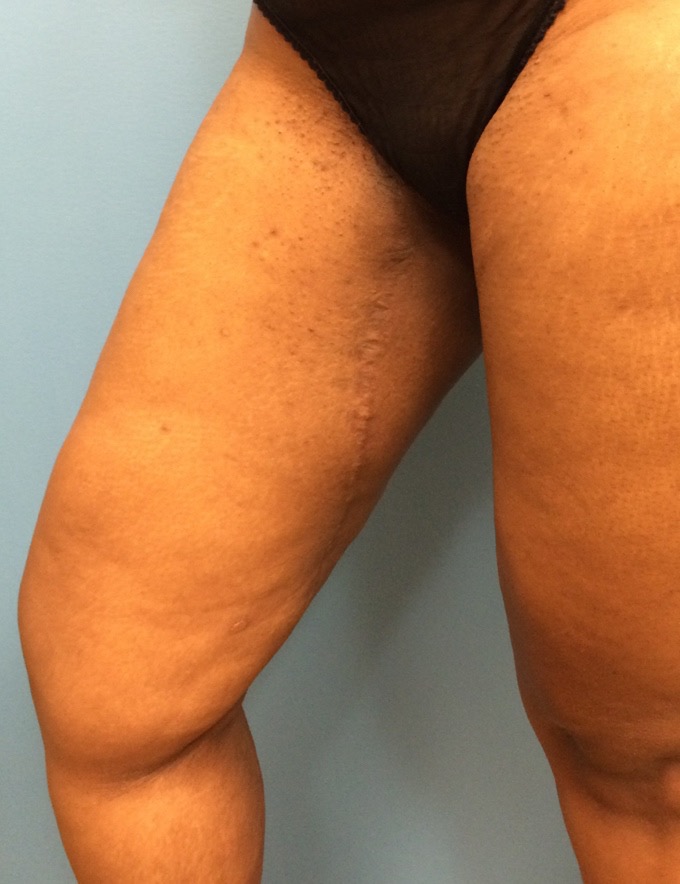
Results: 37 flaps were performed in 24 patients: 3 flaps for partial breast reconstruction, 33 for mastectomy reconstruction. Flap weights ranged from 130-705 grams (average 351 grams). Flap dimension range was 9 x 20 cm to 13 x 25 cm. Average flap width was 10.6 cm. There were no flap losses and fat necrosis was not clinically observed although this was not evaluated objectively. There was only one patient with a small area of cellulitis and superficial delayed healing which resolved spontaneously. One patient developed a donor site seroma with overlying cellulitis treated with percutaneous drainage and antibiotics, and a third patient with donor site cellulitis for a total complication rate of 8.1%. A representative case is shown in Figure 2 & 3.
Conclusion: The DUG flap is a safe and technically straightforward option for patients undergoing autologous reconstruction.
Back to 2015 Annual Meeting
|




