|
|
|
|
|
Back to 2016 Annual Meeting
Long-term patient reported outcomes following unilateral implant breast reconstruction with a contralateral symmetry procedure
Shantanu N. Razdan, MD, MSPH, Andrea L. Pusic, MD, Babak J. Mehrara, MD, Joseph J. Disa, MD, Robert J. Allen, Jr., MD, Joseph H. Dayan, MD, Colleen M. McCarthy, MD, Peter G. Cordeiro, MD, Evan Matros, MD, MPH.
Memorial Sloan Kettering Cancer Center, New York, NY, USA.
Background: A principal aim of postmastectomy unilateral breast reconstruction is to achieve symmetry with the contralateral breast. Unilateral implant reconstruction is often performed in conjunction with symmetry procedures; however, health related quality of life (HRQOL) associated with available techniques is lacking. The study aim is to describe patient reported outcomes following contralateral symmetry procedures including augmentation, reduction, and mastopexy. The hypothesis is that symmetry procedures are associated with improved HRQOL.
Methods: BREAST-Q scores for patients that underwent immediate unilateral implant breast reconstruction with or without a contralateral symmetry procedure were reviewed between 2011 and 2015. Inclusion criteria consisted of patients that underwent a two-stage, expander/implant breast reconstruction with a simultaneous contralateral symmetry procedure at the time of expander replacement. Exclusion criteria involved patients that had revisionary procedures performed prior to their BREAST-Q assessment. Minimum follow-up time was 6 months following the symmetry procedure. Patients were placed into four cohorts: augmentation, reduction, mastopexy and no symmetry procedure. Socio-demographic and clinical variables were recorded. Each symmetry procedure group was compared to the no symmetry group separately. Continuous and categorical variables were compared between the groups using the t-test and chi-square test respectively. Multiple linear regression was used to adjust BREAST-Q scores based on socio-demographic and clinical covariates.
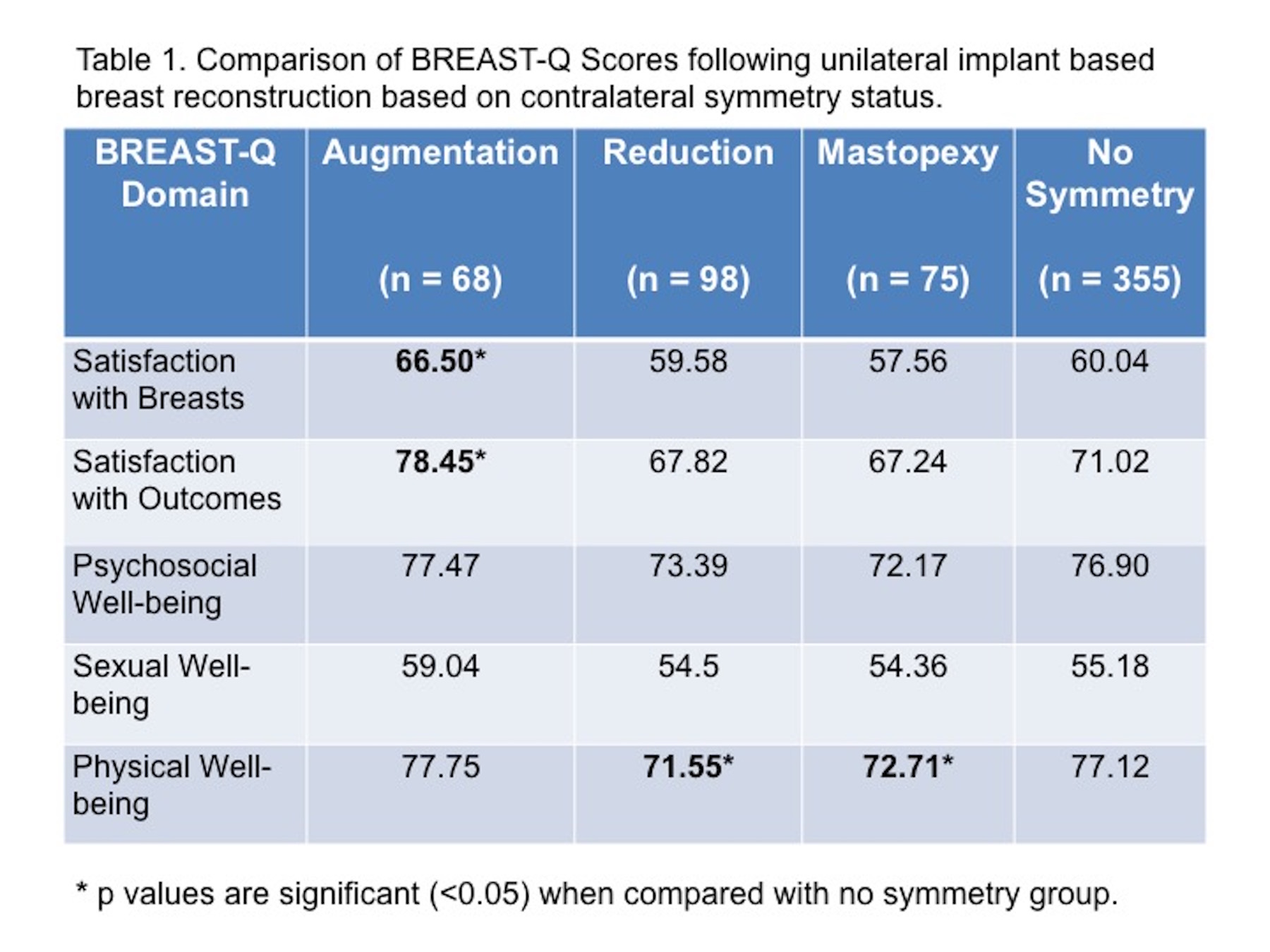
Results: The total number of patients that met inclusion criteria was 596. Contralateral augmentation, reduction and mastopexy were performed in 68, 95 and 76 patients respectively whereas 355 patients did not undergo a symmetry procedure. Mean duration between augmentation, reduction, mastopexy, no symmetry and BREAST-Q assessment was 52, 50, 50 and 48 months respectively (p = 0.81). Scores for each of the six BREAST-Q domains are presented in Table 1. Pair-wise comparison showed that satisfaction with breast and satisfaction with outcomes scores were higher in patients that underwent a contralateral augmentation compared to no symmetry procedure (p<0.05). Physical well-being scores were lower in patients that underwent either a contralateral reduction or mastopexy compared to the no symmetry group (p<0.01). There was no difference in psychological and sexual well-being scores between any of the groups. On regression analysis, contralateral breast augmentation was a significant predictor of satisfaction with breasts after adjusting for baseline covariates (p<0.05).
Conclusions: Patients that underwent contralateral breast augmentation to improve symmetry with a unilateral implant reconstruction reported significantly greater satisfaction with breasts and outcomes compared to those that did not undergo a symmetry procedure. In contrast, breast reduction and mastopexy procedures demonstrated no improvement in satisfaction with breasts and were associated with lower physical well-being scores. Such information will improve the shared decision-making process between patients and plastic surgeons about the HRQOL gains associated with contralateral symmetry procedures.
Back to 2016 Annual Meeting
|
|
